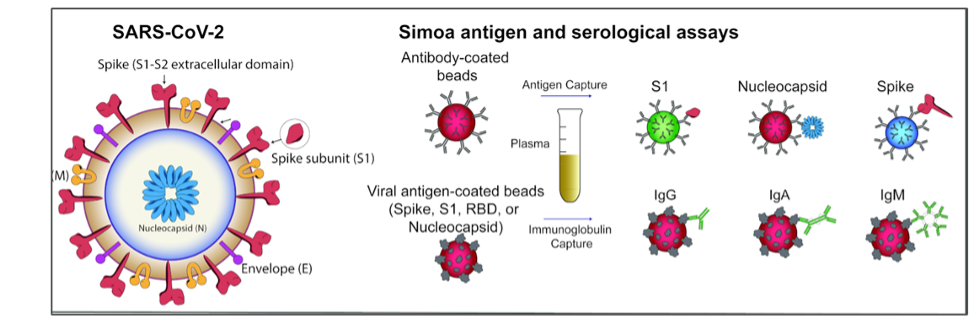
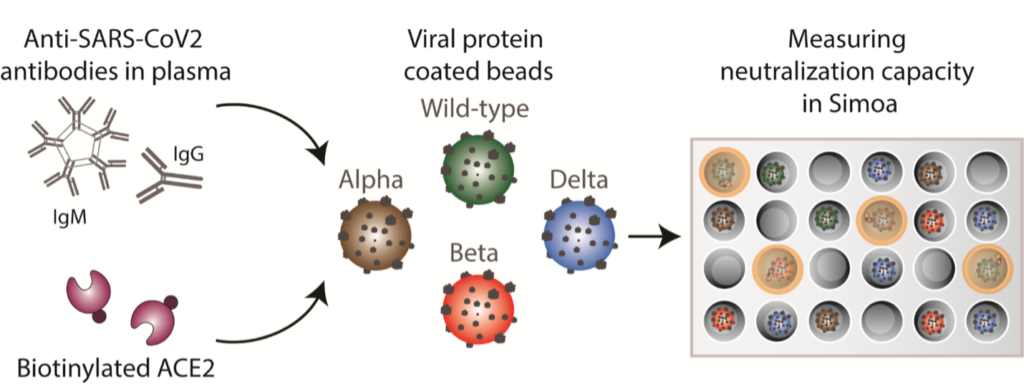
Using the Simoa technology pioneered in our lab, we developed ultrasensitive assays to enable the detection of anti-SARS-CoV-2 antibodies and viral antigens. Recently, we expanded our COVID-19 related technology platforms to include a single molecule neutralization assay, allowing us to measure the neutralization efficiency of an individual’s antibodies against different strains of SARS-CoV-2.
Early in the pandemic, we began by measuring antibody and antigen concentrations over time in plasma collected from patients hospitalized with COVID-19, showing that high levels of viral antigen correlated with disease severity. With the development of novel mRNA COVID-19 vaccinations, we then used our assays to detect circulating spike directly after vaccination and the production of antibodies in cohorts of healthy controls and immunocompromised patients. We are now analyzing plasma from adolescents post-vaccination in an effort to understand why in rare cases certain individuals develop complications, such as myocarditis. In addition, we are studying other illnesses linked with SARS-CoV-2 infection, including multisystem inflammatory syndrome in children (MIS-C), where we discovered high levels of circulating spike persist weeks after SARS-CoV-2 exposure, triggering a severe hyperinflammatory response. We hypothesized that SARS-CoV-2 antigens leak into the blood stream via the gastrointestinal tract due to elevated levels of zonulin, a biomarker of intestinal permeability. Currently, our colleagues at Massachusetts General Hospital are beginning to treat MIS-C patients with larazotide, a zonulin antagonist, and we are continuing to analyze patient plasma samples to study the efficacy of this treatment strategy to reduce circulating antigen levels[WD1] . Given our findings related to MIS-C patients, we hypothesized that adults suffering from post-acute sequelae of COVID-19 (PASC), commonly known as long COVID, may also be suffering prolonged symptoms due to persistent viral reservoirs in the gut or elsewhere in the body. Strikingly, we were able to detect spike antigen in the blood of patients diagnosed with PASC up to 12 months after initial SARS-CoV-2 infection. We are currently continuing this work by analyzing blood samples collected from a larger cohort of PASC patients.
Funding: Chleck Foundation, Amos and Barbara Hostetter, and Mass CPR